
“The Force is what gives a Jedi his power. It’s an energy field created by all living things. It surrounds us and penetrates us. It binds the galaxy together.”
In the galaxy of your body, you are bound together, from every cell to every muscle to every bone to every organ to every nerve by something called fascia. Since everything within you is connected to everything else, that means that your low back pain could be stemming from a restriction in a nearby “planet” like your hip flexors or glutes, or an even more distant satellite like your foot. This continuity has a huge impact on your experience of pain and your ability to perform at your best — whether you are an elite athlete, a weekend warrior, or a just a human being who wants to feel good enough to live the way you want to live.
If you’ve landed on this article you’ve probably heard a buzz about fascia. Perhaps you’re seeking more about the science of fascia or want to know more about the benefits of myofascial massage. Whether your goal is to improve performance or you’re simply seeking some self-care tips, this article will deepen your knowledge and provide a clear understanding of fascia, why it matters, and why properly executed myofascial release is critical to your health and longevity. Scientific research on fascia is expanding weekly, and we will continue to update the information in this article as our collective understanding of fascia grows.
JARGON ALERT
Look for this warning to pop up when we start to describe terms that might seem better suited in a laboratory. We’ll try to give you some manageable definitions that won’t send you running to Google.
Exploring Fascia – Find What Interests You
Click on the links below to be escorted directly to the section that most suits your needs.
The Must-Know Categories of Fascia
What is Myofascia and is it different than Fascia?
What is Self Myofascial Release (SMFR) and How Does it Work?
The Benefits of Self Myofascial Release
Can Self Myofascial Release Reduce Pain?
Can Self Myofascial Release Improve Performance?
Can Self Myofascial Release Improve Mental Health?
What is the Best Way to do Self Myofascial Release?
What are the best Self Myofascial Release Tools?
What is Fascia?
Fascia has long been misunderstood, and it is just now reaching its age of enlightenment . . . finally cracking the dermis into public consciousness and gaining the respect it deserves.
Part of the reason that fascia has been so misunderstood is because it has no particular form. It shape-shifts around your body. It is sometimes firm and fibrous, sometimes goopy. At times it presents itself obviously (as with belly fat), while other times it is hidden, invested like membranous cloaks around the cells within your muscles.
It’s hard to aim the spotlight on a subject that constantly shapeshifts — not to mention how it’s known to “creep” (yes that’s an anatomical term) when it moves… it can’t exactly strut into the limelight on its own. But then, you wouldn’t be able to strut without it. Let’s begin with biotensegrity, a concept that must be understood in conjunction with fascia.
Biotensegrity
The human body is not a mechanistic system of pulleys and levers. It’s what’s referred to as a biotensegrity structure. “An easy way to think about tensegrity is when push and pull have a win-win relationship with each other.”1 Your bones form the compression bearing “struts” and the fascias maintain the tension, leaving your bones “floating” in the fascia.1 In practical application, this means that tension gets distributed around the whole “system of the body.” How does this apply to you? Well, where you are feeling pain may not be the area that needs attention.
Fascia Defined
Fascia is both a tissue and a system… and it only just received an official definition within the last decade.
“Historically ignored, fascia has only recently found some well-deserved respect for its role in mobility and postural integrity. There is even a semi-annual Fascia Research Congress to discuss the stuff.”2
The Fascia Research Congress’s definition of fascia is rather technical:
JARGON ALERT
“A fascia is a sheath, a sheet, or any other dissectible aggregations of connective tissue that forms beneath the skin to attach, enclose, and separate muscles and other internal organs. Definition as accepted by Federative International Committee on Anatomical Terminology (FICAT) See “A fascia and the fascial system.”
The fascial system consists of the three-dimensional continuum of soft, collagen containing, loose and dense fibrous connective tissues that permeate the body. It incorporates elements such as adipose tissue, adventitiae and neurovascular sheaths, aponeuroses, deep and superficial fasciae, epineurium, joint capsules, ligaments, membranes, meninges, myofascial expansions, periostea, retinacula, septa, tendons, visceral fasciae, and all the intramuscular and intermuscular connective tissues including endo-/peri-/epimysium. The fascial system surrounds, interweaves between, and interpenetrates all organs, muscles, bones and nerve fibers, endowing the body with a functional structure, and providing an environment that enables all body systems to operate in an integrated manner. See “Update on fascial nomenclature”
For us non-scientists, here is a more succinct description of fascia from The Roll Model Method, “Fascia is the body’s living aqueous knitting fabric. This seam system is the body’s soft-tissue scaffolding that interconnects you to yourself.”3
Although these seams are continuous, the textures, tensions and purpose of fascia is not all the same. Here’s a quick breakdown of the different categories of fascia.
The Must-Know Categories of Fascia
Watch this video to see the 3 Categories of Fascia
There are 3 main categories of Fascia as of 2019.
- Superficial Fascia (aka areolar or pannicular): It all starts with superficial fascia. Go ahead and squeeze the soft stuff over your glutes or squishy bits around your belly while reading for an “embodied” feeling of fascia. “Superficial fascia lies just beneath the skin and is comprised of loosely arranged areolar (web-like) collagen fibers in a matrix with adipose (fat cells). This layer feels spongy, springy, or fluffy. Ninety-eight percent of your body is coated with fat-filled superficial fascia. In fact, the only area missing the protective fatty cushion in the superficial layer are around the ears, nose, lips, eyelids, labia, and scrotum.”3 Superficial fascia separates skin from muscles, and enables them to glide across each other. It’s also involved in temperature regulation, circulation and lymphatic flow.1 It is peppered with sensory nerve endings that help to provide sensory feedback about various types of touch and pressure to your brain.
- Deep Fascia: Now it’s time to get deep. If you want to palpate while you read, we suggest that you grip the famous band along the side of your thigh. Right about where the stripes on your Adidas pants land is your iliotibial (IT) band, which is a shining example of deep fascia. “Deep fascia (aka) fascia profunda) has a tough duct tape-like appearance, with crimp-like waves in different densities. It is highly organized in its arrangement and is found surrounding muscles or as a thickened, broad,aponeurotic tendon layer.”3 This layer of fascia helps keep everything separate but still connected. It is also the layer where myofascial force transmission occurs across a joint or to neighboring muscles.1
- Loose Fascia: It’s a bit harder to locate loose fascia because it’s more of a “slippery seam” that keeps the layers stitched together. If you’d like to try to get a feel for it, pinch a portion of the flesh on your forearm and try to move it back and forth, up and down… even take it for a spin by winding it up. Pull it up, then let it go and watch it return to the shape of your forearm. Loose fascia refers to fascia that cannot be categorized as either superficial or deep. It is found as an intervening connecting layer between layers of deep fascia, between deep fascia and myofascia, and between superficial and deep fascias. Structurally, it can be web-like or more like a membrane (known as membranous fascia). Loose fascia permits the motion of slide and glide all over your body.”3In 2018 this “loose” zone of fascia spawned another anatomical finding. The term “interstitium” entered the Fascia vocabulary, after scientists observed fluid-filled spaces connecting the body together. They named these spaces, interstitium, identifying them as a conduit of movement throughout the body.4
Jill Miller, co-founder of Tune Up Fitness and author of the book, The Roll Model, helped us understand this concept in a 7/3/2018 post on Instagram:
Fascia: Liquid? Solid? Interstitium? The fascial zones where movement occurs are a true marvel of transitional nature. Here you have abundant fluids, migrant cells, sensory nerve endings, resident cells, pre-lymphatic vessels and plenty of dynamically stabilizing collagen fibers. Their zones exist all over our body and permit differential movement. They are a biological estuary and need to be respected as such. Dr. Neil Theise recently named it the ”Interstitium” and it made headline news worldwide.
For you brave souls open to seeing a cadaver’s fascia up close and personal, you will revel in Gil Headley’s Fuzz Speech video, and will be forever convinced why movement is medicine!
JARGON ALERT
One of the reasons why fascia can be so vexing is exemplified by all of the terms that currently apply to the “loose” fascia layer. It does not yet have a “fixed” name agreed upon by all anatomists. Other terms for this layer are, interstitium, fascial interface, transition zone and Gil Hedley‘s term (one our our favorite anatomists) “perifascial membrane.”
What is Myofascia and is it different than Fascia?
“Myofascia refers to the familiar-named muscle structures along with their associated interpenetrating fascias. For example, your biceps is a myofascial structure, as is your gastrocnemius (calf muscle). There is no muscle that does not have fascia winding its way throughout every layer of its cells and fascicles and surrounding its whole structure. Therefore, while we are in the habit of talking about muscles, the terms myofascia and muscle can be used interchangeably.”3
In other words, myofascia is not “different” than fascia. It is a subset of fascia. Myofascia is a term to distinguish the fascia that is a part of every muscle of your body. Fascia can exist without being a part of a muscle…but a muscle cannot and does not exist without its “myofascia.”
Myofascia = Myo (muscle fiber) + Fascia (the fascial wrappings holding the muscle fibers together to form a muscle)
Muscle fibers are the drivers of mobility and contraction, but they could not function without their fascial partners. The fascia organizes, lubricates and transfers energy for those muscle fibers.2
Myofascia naturally includes the fascia that is cloaking and connecting all muscle fibers together, it “twines around every cell, cell bundle, and group of cell bundles.”3 If you really want to geek out one day you can learn all of the sub-categories of myofascia called endomysium, perimysium and epimysium. We go over these layers in our Tune Up Fitness trainings.
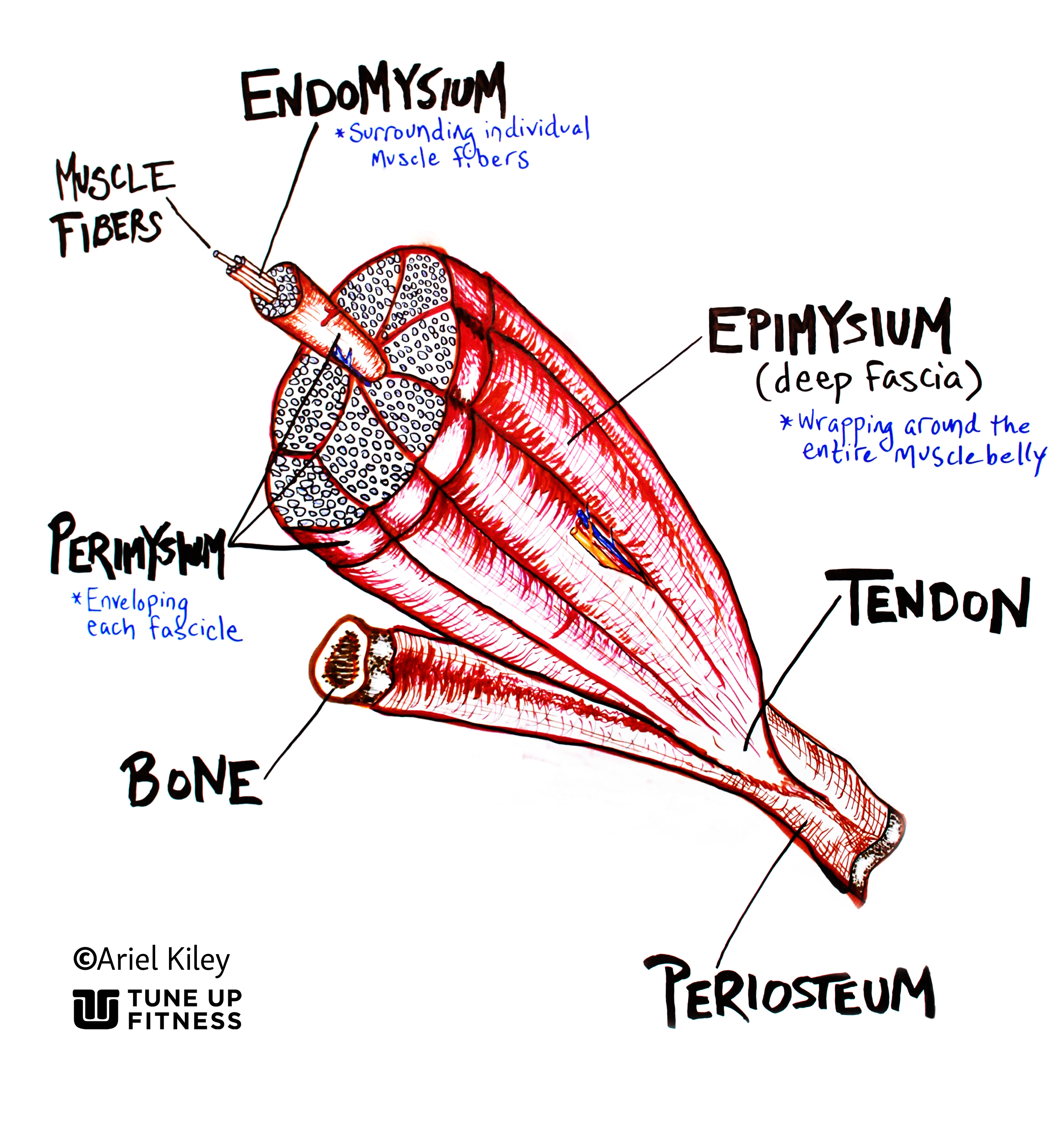
JARGON ALERT
Endomysium: the fascial fibers wrapping around individual muscle cells
Perimysium: the fascial layer wrapping around groups of muscle cells and enclosing them, forming fascicles
Epimysium: the fascial layer wrapping around and enclosing groups of fascicles
Likely the reason “myofascial” gets so much attention, is because seekers of fascial therapies are often doing so related to muscular performance – to improve strength, improve flexibility and improve motor control. But what you must know is that ALL FASCIAS ARE CONNECTED.
Even though we tend to want to separate and categorize in order to better understand the body, fascia doesn’t really work like that.
As David Lesondak explains “The most important thing to keep foremost in mind, at all times, is that the fascial net is one continuous structure throughout the body . . . as far as the body is concerned, the fascia is all one – one complex, holistic, self-regulating organ.”1
When you engage in your rolling practice, take a moment to think about these glistening membranous tissues within you, and let them inform your motion. Indeed, in this zone, the phrase “motion is lotion” is a perfect label.
Indulge in subtle movements and focus on a slow, deliberate touch. Feel how this percolates locally and globally into your whole body sense.
What is Fascia Made of?
Excellent question, here’s where things get really interesting. It is basically both a liquid and a solid. Also known as a colloid.
Fascia is a colloid. Gels and emulsions are colloids. A colloid is a substance that contains particles of a solid material suspended in a liquid. Essentially, a colloid is both fiber and fluid.1
Meanwhile, the components of fascia are cells and the extracellular matrix (ECM).
JARGON ALERT
Extracellular matrix: A complex network of polysaccharides and proteins that provides structure and regulates cell behavior.3
The ECM is both a fiber and a fluid. The ECM fibers are composed of collagen and elastin, and they provide support and structure (the scaffolding) for everything in the body. Collagen, which is the primary protein in ECM, has tremendous tensile strength, which means it can be stretched without breaking. Elastin is an aptly named fiber, as it is very elastic, so it adds additional resiliency to fascia. The ECM is gelatinous soup that fills in all the empty spots in our “inner space.” It’s composed of water and peptides such as hyaluronan, and it’s in this goop where chemical exchanges happen between blood, lymph and tissue cells. This substance is also critical for slide and glide of tissues.1
What are “Fascial Seams”?
While everything is connected to everything in the body, there are certain currents or ribbons of tissue, along which tension and energy are transferred, enabling movement and providing stability. Jill refers to these as “microstitches that compose your weave.”

*Fascial Continuities from Anatomy Trains
These myofascial continuities describe “interlinked series of these connected tracts of sinew and muscle.”5 These continuities are discussed in depth in Anatomy Trains by Thomas Myers, but here is a very brief introduction to seven of the major ones:
- Superficial Back Line – connects entire posterior surface of the body from the bottom of the foot to the top of the head.”5
- Superficial Front Line – connects the entire anterior surface of the body from the top of the feet to the side of the skull.5
- Lateral Line – connects each side of the body from the mid-point of the foot, up the outside of the ankle, the outside of the leg and thigh, along the trunk, under the shoulder, and along the side of the neck to the ear.5
- Spiral Line – loops around the body in a spiral, connecting the one side of the upper body to the opposite side of the lower body, on both the anterior and posterior side of the body.5
- Arm Lines – these lines run from the rib cage and spine through the shoulder and hand.5
- Functional Lines – these lines extend the Arm Lines to the truck and opposite side pelvis and leg.5
- Deep Front Line – this comprises the body’s myofascial core.5
Thomas Myers and Jill Miller have partnered together to provide a self-directed embodied experience of these trains, using the Roll Model Balls. Look for their live events and video collaboration in the summer of 2020! Register here to stay informed.
What is Self Myofascial Release (SMFR) and How Does it Work?
Although the concept of “myofascial release” (MFR) is widely used by the scientist hoping to stake a flag in new anatomical turf, the PT trying to alleviate chronic pain for a patient, or the body-builder aspiring toward a decimal more motor control (and so many more), new research challenges the popularized concept of this term.
“Myofascial release is a term who’s origin emanates from the founder of Osteopathy A.T. Still and his early students. The “release” work uses a therapist’s palpation skills to engage the fascial stretch barrier of a client with appropriate sustained pressure or a variety of manual mobilizations. Conversely, release can be achieved by shifting fascial tissues away from a restriction. In SMFR, an individual performs this tool assisted application in a self-guided manner.”6
Myofascial release can be done as a form of hands-on therapy, as well as a form of self-care. John F. Barnes is a physical therapist who has been using myofascial release and training practitioners since the 70s. He describes this modality as follows:
Myofascial Release is a safe and very effective hands-on technique that involves applying gentle sustained pressure into the Myofascial connective tissue restrictions to eliminate pain and restore motion. This essential “time element” has to do with the viscous flow and the piezoelectric phenomenon: a low load (gentle pressure) applied slowly will allow a viscoelastic medium (fascia) to elongate.
For the purposes of this article, when we refer to “myofascial release” we will be primarily be talking about self-myofascial release (SMFR).
As stated above, we believe it is important to note that the term myofascial “release” (MFR) has recently been proven to be not completely accurate. As you read above, fascia runs throughout your entire body; your nervous system, your vascular system, ALL of your systems sit within it. In a new study that asked whether tissue thickness changed while using a foam roller, it did not find morphological changes in the fascia itself with this particular foam roller application.7 But while the researchers did not find changes in the actual fascial thickness, range of motion (ROM) greatly increased. They also noted that the likely cause of the extra mobility could be from the altered input into the nervous system via sensory receptors in skin, fascia and myofascia, and through changes in fluid dynamics. So, while the term SMFR may not be physiologically accurate, the concept of the practice is vitally important. Further research will eventually explain the exact mechanisms.
MFR is also used to manipulate scars and the adhesions associated with them. The scar tissue can alter mechanics far away from the site of surgery or injury even after the body’s fascia has repaired itself. The scar represents an agglomerate of solidified fluids and fibers that acts as a new more stable tissue where those same tissues were once breached.1
JARGON ALERT
Morphological: having to do with the form of structure of something
Agglomerate: when things collect or form in a mass group (such as when fascial tissues and fluids stick together in a mass, cluster, adhesion or scar)
Adhesion: fibrous bands that form between tissues and organs, often as a result of injury. They may be thought of as internal scar tissue that connects tissues not normally connected.
The Benefits of Self Myofascial Release
Do you want to move with power and grace? Experience less pain and more peace? Are you looking for faster muscle recovery?
Self myofascial release (SMFR) has been proven to facilitate all of these things. SMFR has many of the same benefits as manual myofascial release, with the added benefit that they can be done on your own terms, at your own convenience, and for free! Also, for people who are touch-adverse, SMFR provides a way to get the extensive benefits of MFR as well.6 Let’s explore these benefits more fully.
Can Self Myofascial Release Reduce Pain?
Self myofascial release can reduce pain in the body via several different avenues. It’s an effective remedy for both acute pain and chronic pain. Here are a few key elements:
- Release Trigger Points: Pain can be caused by trigger points, which are “a hyperirritable spot in skeletal muscle that is associated with a hypersensitive palpable nodule in a taught band.”8 These trigger points can cause pain, tenderness, motor dysfunction and autonomic phenomena in the trigger point itself and in a referred area.8 These areas of hypersensitivity can be addressed with SMFR.
- “Pain caused by myofascial trigger points (TrPs) may present as an acute, recurrent, or chronic pain syndrome. In the presence of sufficiently severe perpetuating factors, an acute syndrome persists to become a chronic myofascial pain syndrome.”9 When unresolved, trigger points can persist and cause secondary and satellite trigger points, leading to widespread and chronic pain. Addressing trigger points and other perpetuating factors such as postural patterns and joint dysfunctions can help address chronic myofascial pain.9
- Enlighten Your Homunculus: Your body is mapped to a portion of your brain called the sensory motor strip which provides a representation of how much cortical real estate (brain sensation function) each body part receives (the neurological term for this is Homunculus). These “body maps” are consistently updated by changes in bodily sensation and action. When information is not clearly relayed from the body to this area of the brain, there can be “blurry” areas in the “body map” that can play a role in pain, tension and sub-optimal movement. SMFR may be able to provide sensory input that may assist in the accurate refinement of these “body maps”, especially when combined with movement, breathwork, and posture exercises.21
- Improve Proprioception: Proprioception is “Your body’s sense of itself. Your inner GPS system. The ability to sense the position, location, orientation, and movement of your body and it’s parts.”3 As mentioned above, improved proprioception can help decrease pain by improving the cortical map. By stimulating various sensory nerve endings in the fascia, SMFR serves as an avenue for improving proprioception and identifying areas that are misused, abused, or confused. In Yoga Tune Up®, we call these “body blind spots.” By identifying and exploring these body blind spots, your perception of pain can be diminished.
- “One biological fact of utmost importance is that there is a mutually inhibiting relationship between pain (nociception) and proprioception (body sense).3 The more proprioceptively aware you become, the higher your ability to manage pain.
JARGON ALERT
Various mechanoreceptors associated with proprioception are stimulated with SMFR, including muscle spindles, golgi tendon organs, Pacinian corpuscles, Ruffini endings, and interstitial fibers.3 Different receptors are located in different depths with your body and within different types of tissues: muscles, tendons, ligaments, joints – all the way down to the periosteum of bone.3 These sensory nerve endings have different effects on the body when stimulated, such as reducing muscle bracing, lengthening myofascia, releasing tension, and they are stimulated in different ways (rapid pressure, slow pressure, sustained pressure, stretch, etc.), which is the basis behind The Roll Model Techniques.3 For more information on this topic, please see pages 112-113 of TRMM.
Can Self Myofascial Release Improve Performance?
It would almost be quicker to list how MFR DOESN’T improve performance! But, just to really drive home the point that YOU SHOULD BE DOING SELF MYOFASCIAL RELEASE, we will give you all the juicy details. Here is a sampling of what SMFR can do for you: improve movement coordination, improve joint range of motion and mobility, increase torque, decrease muscle fatigue and soreness, reduce arterial stiffness, improve vascular endothelial function, decrease lymphedema, improve slide and glide of tissues and fluid dynamics.6 (additional references within)
So SMFR is a vital tool that should be used by athletes to enhance their performance, as well as by weekend warriors who don’t want to groan loudly when they try to stand up from their chairs after their first Monday morning conference call.
- Pre-covery and Recovery – SMFR is a key component to both preparing the body for efficient movement and for helping the body recover afterwards. Two studies done by Dr. Robyn Capobianco showed that rolling the gastrocnemius on a soft rubber Yoga Tune Up® ball was able to offset a stretch-induced force deficit, while also increasing torque, range of motion, and force production. These results were demonstrated by both college and middle-aged adults. The results for middle-aged adults were extremely interesting, as their ankle dorsiflexion (the lack of which often drives slip and falls) increased by almost 25%!13, 14
- Improved slide and glide – Our layers of tissues are meant to slide and glide across each other, enabling effortless, graceful movement and free-flow of life-giving fluids throughout the body. However, when we hold our body in a static position for several hours a day, several days a week, fascial changes start to occur. The layers of tissues start to adhere to each other, and fascia starts to become dense and fibrotic. Fascial restrictions can lead to: restrictions in the flow of lymph and blood. Remember – 90% of fluids are reservoired in the fascia!
- Muscles that are unable to fully contract or stretch, leading to imbalances throughout the body and restrictions in proper joint mechanics.3
- Nerve compression, resulting in “tunnel syndromes” where the nerve gets compressed within the fascia, causing inflammation and sensitization inside the nerve itself.15
- Chronic pain conditions like fibromyalgia. SMFR can help people suffering from chronic pain by reducing stiffness, fatigue, wide-spread pain intensity and ROM.16
Elite athletes have teams of therapists who work with them to keep their tissues functioning optimally and to balance out the effects of intense training. However, for the executive who loves to hit up the links every weekend, or the retiree who lives to obliterate the competition on the pickleball court, or the bank teller who recently started Crossfit – SMFR can help these every-day athletes keep their fascia healthy, hydrated and pain-free.
Can Self Myofascial Release Improve Mental Health?
Just like everything is connected to everything via fascia in the body, the mind and the body are also inextricably linked. The mind and the body are two sides of the same coin. This fact is recognized in the biopsychosocial model of pain. This model states that there can be biological and biochemical contributors to pain (e.g. a broken leg), as well as psychosocial contributors to pain (e.g. depression, anxiety, loneliness, stress, etc.). All of these inputs are processed by the nervous system, which decides if all incoming signals should result in an outgoing pain signal. Pain is an experience in the body, and it often presents itself even when there is not physical tissue damage, and sometimes there IS tissue damage, but NO pain!
JARGON ALERT
Biopsychosocial model of pain: The biopsychosocial model is an interdisciplinary model that looks at the interconnection between biology, psychology, and socio–environmental factors. The model specifically examines how these aspects play a role in topics ranging from health and disease models to human development. – Wikipedia.
SMFR can help down-regulate the “biology” portion of the pain experience, as described above.
But, perhaps even more importantly, it also positively affects the psychosocial component.
Self myofascial release/SMFR is a ticket to physiological relaxation, increased parasympathetic activity, and improved embodiment. This ties in to the discussion about proprioception above. But it also opens up another conversation into another subtle category of sensing our body’s implicit feelings called interoception. Interoception is our body’s physiological sense of itself, the many nerve endings that comprise this aspect of body sense are also embedded in our body’s fascia, but our brain processes the majority of these signals in its emotional processing centers.10 By stimulating all of those various nerve receptors while doing SMFR, your brain is getting a much clearer map of your body.
SMFR can also facilitate an improved awareness and emotional connection with the inner Self. When the human organism experiences trauma (which can include falls, car accidents, surgeries, and other more complex forms of trauma), and the trauma or “threat” is not processed successfully, the energy mobilized by the body to deal with the threat can get trapped in the body, causing constrictions and a host of other symptoms such as panic attacks, anxiety, difficulty sleeping, chronic fatigue, headaches, digestion challenges, neck and back problems, depression, forgetfulness, inability to deal with stress, etc.11
Interoception can help humans be present and aware of the sensations, emotions, and feelings flowing through the body. Building this capacity to be present with what is happening in our “inner space” can help the body process the stuck energy mobilized by trauma.12 When practicing SMFR, give yourself permission to BE in your experience – to be curious, open, patient, to go s l o w. Notice how the pain experience changes with different thoughts, different movements, and different and novel experiences. Be open to witnessing your rage of emotions. Be a companion to the pain instead of fearing and resisting it.
*This content is not intended to be a substitute for professional medical and psychological advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding any condition.
JARGON ALERT
Interoception: a subtle sensing system of how we perceive our body’s physiology. Interoceptive signals include hunger, visceral pain, cramps, sexual desire, breath, heart beat etc.
What is the Best Way to do Self Myofascial Release?
You might also ask, is there a wrong way and a right way? Well, the short answer – Yes! When exploring your tissues with self-massage tools, do so with curiosity, awareness, patience and gentleness. Your goal with SMFR is to soothe your tissues, to encourage them to return to a restful tone – relaxed and balanced, yet ready for action. It doesn’t have to hurt to work!
You don’t have to grind down your soft-tissues to get them to lengthen, soften, or loosen. In fact, the more you bully your soft tissues, the more you arouse their innate defense mechanism. They brace in response to threat, via the muscle spindle response. Guess what else braces? Other nearby muscles who rally to protect the tissue under attack.
The more you push, the more they push back. So when you’re rolling yourself like you’re ironing your birthday suit, your fascial tissues will likely swell and inflame full of defensive cytokines and make you feel even more swollen & stuck than before. Often as you roll, or stick or whatever, the “ouch” that you feel is your nervous system kicking into high gear and telling you that you’re pushing too hard, and to please back off. Are you listening? Or BALLdozing through it? — Jill Miller
In the Roll Model® Method, we use 9 primary techniques for optimal SMFR, they include:
- Sustained Compression: Allow the Therapy Ball to rest without movement as you apply consistent pressure to one area
- Stripping: Slide a ball (or pair) from one end of a muscle area to the other, combing through both the superficial and deep fascial layers going back and forth (from origin to insertion)
- Cross Fiber: Move, slide, or drag the Therapy Ball across the “grain”of a muscle to mobilize multiple layers of fascia
- Skin Roll/Shear: Use a Therapy Ball to gently pinch your skin as you traction and shift your superficial fascia over the deep fascia
- Contract/Relax: Dock the Therapy Ball on a spot, stiffen the muscle where the ball is placed and hold for seven to 10 seconds, then relax
- Pin & Stretch: Pin a Therapy Ball anywhere along a muscle and move a joint that is above or below while keeping the ball locked in place
- Pin/Spin &Mobilize: Put the Therapy Ball on a target within muscle, twist it into that spot, then move a neighboring appendage away from that spot keeping the ball pinned
- Plow: Move the ball(s) like a squeegee to gather as much of the loose fascia as possible and move it as a mass in one direction
- Stack: Place one Therapy Ball underneath the area you want to address and place another ball on the opposite side of that area then apply pressure to both sides simultaneously
Watch our video playlist of these self myofascial techniques and download our Roll Model SMFR Techniques Poster for a handy reference of each technique.
As mentioned, the human body is a biotensegrity structure, so stress and strain gets transferred across the system. Consequently, when doing SMFR, it’s important to investigate the “peripheries” of where you are feeling pain. If your upper back hurts, explore your neck and pecs. If your knee hurts, roll out your calves and feet. This relates back to the Fascial Seams previously discussed.
Often, “the loser complains,” meaning that the muscles that are getting stretched (eccentrically lengthened) are the ones sending nociceptive signals to the brain, but it’s really the muscles that are hypertonic/contracted that need to be addressed. So, explore uptown, downtown, and around the town to see what is really going on throughout the whole neighborhood! Remember, with fascia, everything is an interconnected system. As you go through this process, you’ll likely discover silently suffering areas of chronic tension, a.k.a “body blind spots.”
Use the Roll Model therapy balls to root out these blind spots, and administer the techniques above to fluff, stimulate and traction these tissues; in the process you’ll empower your self-care skills and become one of your very own healthcare providers.
What are the best Self Myofascial Release Tools?
The goal is to treat your tissues with the respect they deserve – i.e., treat your tissues well and they will serve you well in return. Given that, should you batter them into submission with the edge of a kettlebell? Plow the pain out of your IT band with a hard foam roller? Find an edge of a window sill and get into the stabbing pain by your shoulder blade?
Fortunately Science has provided an answer! In a study conducted in Korea by Yushin Kim et al, researchers discovered that therapeutic tools providing gentle pressure are superior to those providing firm pressure. In the study, the researchers used a soft inflatable rubber ball to massage the posterior neck muscles. The soft rubber ball resulted in reduced muscle tension and discomfort as well as increased neck extension ROM and decreased tissue thickness.17 Another study showed that a softer tool increased mechanical stress transfer to the targeted tissue, which is the avenue by which massage has so many beneficial effects.20
Harder tools create a threat response – causing muscles to brace against the intrusion, inflammation to increase, and increasing stress hormones like adrenaline and cortisol. Using a harder massage tool can also increase the risk of injury. In a May 2019 case report, a woman injured the tibial division of her sciatic nerve by massaging her glutes with a lacrosse ball.18
Like Likes Like – the human body reacts best to being touched by something similar in texture, density, and hardness to itself. “Your soft tissue likes a soft tool.”3
One of the reasons we developed the Roll Model Therapy Ball products is because they have an inner density that maintains integrity but are surrounded by a soft, pliable and grippy outer layer. This grip helps grab multiple layers of fascia, enabling you to perform all of the key techniques that effectively stimulate mechanoreceptors without creating muscle bracing or damaging soft tissue.
Now, It’s Time to Get Started…
Thanks for sticking with us on this epic journey through the gorgeous galaxy that is your human body. You now know what you are really made of and how to take care of your fascia and myofascia. The body is meticulously woven together, cell-to-cell, to perfectly adapt to how you use it. However, sometimes those adaptations, based on how we use (or misuse) our body, can begin to cause pain or restrict mobility.
With the knowledge of fascia and your new self myofascial release skills you can slowly remodel your tissues to facilitate a better flow of body and mind. Couple that with the proper soft tissue tools, time, patience, and curiosity, and you have the power to decrease pain, improve performance and mental health, and elevate awareness of your inner space. You now know what tools to use, and how to use them. If you’d like an even deeper study, consider taking a Tune Up Fitness Training and see Jill Miller’s new book Body by Breath. May the Force be with you!
References
- Lesondak D. Fascia: What It Is and Why It Matters. Edinburgh: Handspring Publishing; 2017.
- TBiel A. Trail Guide to Movement: Building the Body in Motion. Boulder, CO: Books of Discovery; 2019.
- Miller J. The Roll Model: a Step-by-Step Guide to Erase Pain, Improve Mobility, and Live Better in Your Body. Las Vegas: Victory Belt Publishing; 2014.
- Benias PC, Wells RG, Sackey-Aboagye B, et al. Structure and Distribution of an Unrecognized Interstitium in Human Tissues. Scientific Reports. 2018;8(1). doi:10.1038/s41598-018-23062-6
- Myers TW. Anatomy Trains. Edinburgh: Churchill Livingstone/Elsevier; 2009.
- Fascia, Function and Medical Application, edited by David Lesondak, Jill Miller et al, Taylor and Francis ahead of Publishing.
- Yoshimura A, Inami T, Schleip R, Mineta S, Shudo K, Hirose N. Effects of Self-myofascial Release Using a Foam Roller on Range of Motion and Morphological Changes in Muscle. Journal of Strength and Conditioning Research. 2019:1. doi:10.1519/jsc.0000000000003196
- Travell JG, Simons DG, Simons LS. Myofascial Pain and Dysfunction: the Trigger Point Manual: Vol. 1:Upper Half of Body. Baltimore: Williams & Wilkins.; 1999.
- Travell JG, Simons DG, Simons LS. Myofascial Pain and Dysfunction: the Trigger Point Manual: Vol. 2:The Lower Extremities. Baltimore: Williams & Wilkins; 1999.
- A.D. (Bud) Craig. How Do You Feel? An Interoceptive Moment with your Neurobiological Self
- Levine PA. Waking the Tiger: Healing Trauma: the Innate Capacity to Transform Overwhelming Experiences. Berkeley, CA: North Atlantic Books; 1997.
- Blackstone J. Trauma and the Unbound Body: the Healing Power of Fundamental Consciousness. Boulder, CO: Sounds True; 2018.
- Capobianco RA, Almuklass AM, Enoka RM. February 2018. Manipulation of sensory input can improve stretching outcomes. Eur J Sport Sci. 18(1):83-91. doi: 10.1080/17461391.2017.1394370.
- Capobianco RA, Mazzo MM, Enoka RM. February 2019. Self-massage prior to stretching improves flexibility in young and middle-aged adults. J Sports Sci. 4:1-8. doi: 10.1080/02640414.2019.1576253.
- Jacobs D. Dermo Neuro Modulating: Manual Treatment for Peripheral Nerves and Especially Cutaneous Nerves. Victoria, British Columbia: Tellwell; 2016.
- Ceca D, Elvira L, Guzmán JF, et al. Jul-Aug 2017. Benefits of a self-myofascial release program on health-related quality of life in people with fibromyalgia: a randomized control trial. J Sports Med Phys Fitness 57(7-8):993-1002.
- Kim Y, Hong Y, Park HS. 2019. A soft massage tool is advantageous for compressing deep soft tissue with low muscle tension: Therapeutic evidence for self-myofascial release.
- Cho JY, Moon H, Park S, Lee BJ, Park D. Isolated injury to the tibial division of sciatic nerve after self-massage of the gluteal muscle with massage ball. Medicine. 2019;98(19). doi:10.1097/md.0000000000015488
- Pearson N, Prosko S, Sullivan M. Yoga and Science in Pain Care: Treating the Person in Pain. London: Singing Dragon; 2019.
- Blyum L, Driscoll M. Mechanical Stress transfer – the fundamental physical basis of all manual therapy techniques. Journal of Bodywork and Movement Therapies. 2012;16(4):520. doi:10.1016/j.jbmt.2012.01.006
- Medina J, Coslett HB. From maps to form to space: Touch and the body schema. Neuropsychologia. 2010;48(3):645-654. doi:10.1016/j.neuropsychologia.2009.08.017

![New to Self Massage? Start here! Self Myofascial Release Techniques Using Massage Balls [button]](https://www.tuneupfitness.com/wp-content/uploads/2023/07/SelfMyofascial_Blog_Journey_Button.png)









OMG. This article was fantastic. I teach yin yoga & so am familiar with fascia. However, your through explanation of the types, the connections a the self-release methods was the best I’ve read. Now I have to read Lesonda’s book. Is there a way I can save this article? Thank you, thank you.
Wow! Some much information broken down, simplified and in one place. Thank you! There are so many benefits to self myofascial release. My favorites are the peace it brings me and the connectedness to my body.
Such a gift!
Thank you, Heather, for such a comprehensive article! I first became acquainted with fascia and self-myofascial release about a decade ago when my Pilates instructor returned from a body dissection workshop in the USA with Tom Myers. She was so excited and began sharing her insights with us, introducing a strong focus on fascia in our Pilates sessions and body embodiment practices. I loved it so much that I began researching and learning about fascia on my own.
A pivotal moment came on my 52nd birthday in February 2019, when I had the opportunity to attend Dr. Antonio Stecco’s body dissection presentation at Tel Aviv University in Israel. The event was open to professionals who typically don’t have access to body dissections, and it was truly a life-changing experience.
From there, I continued my learning journey and discovered Jill Miller online. I immersed myself in her self-paced courses, completing almost everything she offered. Then, last year, I participated in Rolling Along the Lines, a course by Jill Miller and Tom Myers, which was incredibly educational and revealed several blind spots I hadn’t been aware of.
Most recently, in November, I completed the Yoga Tune-Up teacher training course. This experience deepened my understanding of my body, mind, and soul, uncovering even more blind spots that I’ve now committed myself to explore further.
Thank you, Jill, for guiding me on this transformative journey and for providing such valuable tools and knowledge along the way.
This article is an exceptionally thorough and clear resource. I will be sharing it with students and clients! I appreciate the reference to Gil Hedley’s phenomenal work; no words can replace the visuals (if one is up for seeing the tissues). I absolutely love Jill’s “seam system” imagery and the phrase “microstitches that compose your weave.” YES! And omg the phrase “enlighten your homunculus” makes my whole body smile… EmbodyMap is where it’s at :~D
Fabulous detailed article!
– I’ve learned about many of these concepts within occupational therapy such as biotensegrity with hand therapy, proprioception and interoception within sensory, fascia within the muscle and have always had an inner knowing that everything was connected but to finally feel like I’ve finally put my finger on it, to find the secret ingredient that has it all make sense.
For this, thank you!
Thank you for this detailed and accessible article on fascia. I recall learning anatomy on cadavers years ago, where we removed the fascia, treating it as little more than excess tissue obscuring the essential structures. How times have changed! Who would have thought it would become recognized as a key component in both physical and mental health?
This article clarifies how fascia connects everything in the body and how restrictions in one area can impact others. It’s fascinating to think that low back pain could stem from tension in a distant muscle! Thanks for sharing the importance of myofascial release in maintaining overall mobility and reducing pain.
The use of elastic bands to explain the layers of fascia is brilliant. Once seen, never unseen. It was the video that really made me realise the interconnectedness of every part of the human body. So having a pain in one part of my body is never just about that part of the body, but the upstream and downstream of it is important too. I was thinking of this in relation to how we medicate for a symptom. It seems very unidimensional to not consider the global factors (the upstream and downstream) that can lead to a symptom. Learning about fascia has truly led me to see the body in its “whole-ness” rather than as bits that make up a “whole”.
Oh wow! This is a true treasure trove of knowledge about fascia. Ever since I started learning about fascia, I’ve been surprised at how little attention this topic receives. I feel that many doctors and physiotherapists often lack this knowledge. Personally, working with fascia has been a game changer for me. Self-massage before a yoga practice or after a long day helps me so much. Our bodies are truly amazing.
Self myofascial release is a topic that has interested me for probably 15 years, although so much of what we understand about fascia is so much newer than that. I bought my first foam roller probably 15 years ago, back when I knew relatively nothing but knew that when I used it for self myofascial release, I simply felt better in my body. I’ve done a lot of reading and taken several courses on self myofascial release – including the Roll Model Method, which is excellent, and Rolling Along the Anatomy Trains, which was both educational and delightful. I still feel like I have so much to learn.
I have led a number of workshops on self MFR, and one thing I try to emphasize is how everything is connected – pain in a specific part of the body may not actually originate there. People are always surprised at how when they roll their calves, for example, that their lower backs may find relief. It truly is wonderful watching people’s faces when they realize it in their own bodies. I also love how accessible and non-intimidating it is for people, and how learning how to manage their own pain/discomfort empowers them.
I am so excited to continue my learning about techniques and benefits, and keeping up on the latest research. It can be life changing, for sure.
I really enjoyed this article! It was very helpful to get an explanation of the interstitium. I am a healthcare provider and it is often brought up especially in terms of fluid balance, but without any explanation of what that means other than “tissue.” The details concerning what the interstitium is was very helpful in appreciating the concept. I also am very interested in the anatomy trains and learning those. I got a much better appreciation of the concept that fascia connects everything to itself in the body!
I absolutely love using the Corgeous Ball. I first used it on my stomach and was literally shocked at how much tension there was in my tissue. Especially in the area where the organs are attached, even carefully breathing into the ball caused a noticeable response. After 20 minutes of breath work and gentle massage, the tension was noticeably relieved, my stomach circumference even decreased and my digestion got going. To this point, I found it very difficult to extend yogic breath over long beats (I ran out of breath relatively quickly).
After just a few abdominal massages, breath working und contract-relax-technique, I was able to noticeably lengthen and better control my breath. What an overwhelming experience!
It is really interesting that different modalities use divergent methods but have similarly profound effect on fascia. For instance, with ELDOA, the basic spinal ELDOAs create a position that fix the inferior articular segment while mobilizing the segment above. This position is created to place ALL inferior and superior myofascial chains under tension. Both ELDOA and the modality of using yoga tune up balls are sometimes uncomfortable. ELDOA focuses on strengthening through isometric movement while the use of the tune up ball is generally to loosen up tight areas in myofascia, reduce adhesions, etc. I think that both are necessary for optimal movement and good health.
This is one of my go-to blog posts when I try to help people understand the fascial system better. This is robust and even with the more scientific jargon (which I personally love) is accessible and easily comprehended. The videos are add a nice complement to the text to better visualize and sense what is being discussed. I loved when Jill said, “Work local – Get a Global Response!”
Thanks for pointing out that a myofascial release can also help me stretch more easily. I’m interested in looking for a good myofascial release therapist because I want to start training for a marathon soon. Being able to make sure that my body will be ready for that will be crucial in the long run.
Great article. Thank you for all the fascia info. From experience using the YTU balls for SMFR, it is amazing how rolling one area of the body releases so many other areas and the positive impact it has on pre & post training as well all of your everyday activities
This work is truly magic. I found myofascial release after having my first C-section about 16 years ago. At that time, I hadn’t found YTU yet, but was immediately hooked. Anytime I had a strange pain that wouldn’t go away with normal rest or stretch (usually from running), my MFR guy could melt in away in 1-2 sessions. Since then, I’ve been a fangirl of YTU and MFR because it allows me (and anyone) to address their pain and postural habits in was that empowers overall health.
I really loved this article and its in-depth and accessible explanation of fascia. I heard recently that if all your organs and other tissues were removed and only your fascia remained, you would still look recognizably like you, which blew me away. I’m amazed buy the different states that fascia can manifest as, such as loose, deep and superficial. I didn’t know that it was considered a colloid, or liquid solid, which I think is so cool! In another training this summer it was referred to as closer to plasma than a fibrous tissue. I also like the idea that the fascia holds the stories of our bodies within it, like a record of who we are that we can access with palpation, movement, breath, and other practices. Now I understand how craniosacral unwinding works by tuning into the fascial pathways and seams, which is super cool thinking that’s what I’ve been feeling in my hands in my bodywork practice this whole time!
Thank you for a nice summary of fascia. I have a few questions: I am confused by the definition of fascia as a dissectible aggregation of connective tissue while at the same time being “a living aqueous knitting fabric” that is both liquid and solid. I agree that connective tissues found on the outside of cells are composed of proteins and fluid but I m having difficulty with dissectible aggregation as part of the definition. Does this mean that connective tissue that can not be dissected in not considered fascia?
I was intrigued by the statement that pain and proprioception are mutually inhibiting and wondered if you can tell me more?
Thank you!
Super!
Super article pour une meilleure compréhension du fascia! Et cette compréhension est indispensable pour mieux vivre.
Super article qui explique avec des mots simples l’univers du fascia, du massage par balles tune up. Cet article va beaucoup m’aider à amener de la compréhension sur ce sujet à mes élèves . Il sera un outil formidable pour m’aider à transmettre ma passion des balles thérapeutiques. Merci
Présence accrue des fascias dans notre corps….certes oui! Ayant eu un accident de vélo et subie une déchirure de l’acromion qui a fait que ma clavicule a percé la peau de mon épaule , je suis très consciente de l’importance qu’il faut accorder aux fascias afin de retrouver les directions de mouvements que j’avais avant l’accident. Le massage des muscles dans cette région à été d’une aide grandiose pour ma réhabilitation.
Maintenant, j’accorde encore plus d’importance aux fascia dans mon corps afin de conserver et améliorer mon état.
It is all interconnected: “all fascias are connected… As David Lesondak explains “The most important thing to keep foremost in mind, at all times, is that the fascial net is one continuous structure throughout the body . . . as far as the body is concerned, the fascia is all one – one complex, holistic, self-regulating organ.”1
Article fascinant sur les fascias, lorsqu’on se rend compte de ce que cela apporte dans notre santé globale on ne peut qu’être passionné par les fascias. C’est un kiné qui m’a fait découvrir les fascias en 2016, lorsque je suis allée le voir pour des soins. Son travail sur mes fascias a été le début de la délivrance de mon corps qui souffrait quotidiennement. Merci pour les références apportés dans cet article qui vont alimenter ma curiosité.
I love how in depth this article goes into the discussion of fascia! As a student of the body there’s nothing more important to me than feeling included in the conversation I’m trying to learn. Also, I really appreciate all the extra resources offered on this subject! The Fuzz speech is the holly grail to all my questions when it comes to fascia and why we use the self myofascial release in the first place. I’m excited to continue to learn more about this rather “new” discovery and invite more people to join the conversation!
I really enjoyed this amazing article on mysterious and fascinating fascias!Understanding the fascias allows us to understand our body and its health in a more global way.Thank you!
Thanks, this blog post gave me new language and exciting ways to explain and teach my clients about their fascia and fascia restrictions. I enjoy the phrase “motion is lotion” and will continue to use that in my own myofascial release practice and with clients.
Love the easy to understand language of our largest and most important connective tissue! The “fuzz” video was so informative. Every detail and explanation in this article is consumable and blew my mind! Loved deepening my understanding of fascia, myofascia and SMFR. Thanks for the fantastic information.
I had no idea that fascia is both a fibre and a fluid, as I assumed it was fibrous material only. I’m happy to see the reference to anatomy trains as well given the topic. It’s fascinating how connected everything is and how one spot of pain may not have anything to do with the area itself, rather another area altogether. So, it’s also really fascinating when my massage therapist works on my ankles and wrists and all of a sudden I have more movement elsewhere on my body. I’m on a new journey of finding body blind spots on my own rather than always having to go to a functional or movement therapist; now with learning proper rolling techniques, I can explore this on my own, at my own pace.
Thanks for this great article.
This article gives you all the basics and fundamentals about fascia and self-myofascial release that anyone without much prior knowledge in anatomy would still be able to comprehend. The word myofascia often causes people to tune out from the next things you’re trying to say to them, as it is still rather a never-heard-before word for many people and induces an impression of complicated anatomical subject. Therefore I changed my strategy and started sharing the image of sub-categories of fascia by Ariel Kiley and coupling it with “orange dissection” (The Roll Model book pg 105-106) to explain myofascia to my workshop participants. It is so heartwarming to see them “get it”. So do yourself and your students a favor by utilizing the information provided in this article to enrich your knowledge with this fascia-nating science.
Fascia is amazing!!!! And a colloid, which I had never heard of. I love the image of a solid material suspended in a liquid and picturing that all over the body! Like all over! And although I am not super familiar with the fascial anatomy trains, I love tracking the sensations and feeling the connections in my own body!
Would you agree that the shift from a biomechanical understanding to a biotensegrity understanding is an enormous paradigm shift? Do concepts such as agonist/antagonist pairs and exercises targeting certain muscle groups become obsolete in this new paradigm? or even the concept of stretching? If we are comprised of biotensecritic structures, then stretching is not really happening, but rather the whole organism is responding to pressure or tension and moving in response to that pressure/tension? It’s not black or white, but sometimes i wonder about continuing to talk from a biomechanical perspective is no longer so useful. What is your opinion?
My mind was blown by the video explaining the “fuzz!” It’s remarkable to learn how the body behaves on a cellular level. If there is an injury or someone doesn’t have great movement patterns, is the build up of fuzz reversible or at a certain point is it almost acting like scar tissue?
This information makes me want to get up and stretch right now!
Thank you for this exhaustive and clear article on the fascias and their maintenance for our health and longevity. You beautifully present all the many benefits of SMFR and the various gentle, non-intrusive massage techniques for the nervous system!
Thank you for that expose on fascia and myofascia. it is very comprehensive and complete. I will certainly have to come back and read it again and again.
I can’t wait to read more about fascias, especially fascia seams. It is really a source of wonderment to me.
Very interesting article, I have been interested in fascia for several years but more this post year. It is very interesting to see in one of the videos how the fascia detaches more or less easily depending on its degree of thickening.
Thé PDF will be so Yelp full tks.
There is so much to learn about the fascia! I shared this text with my dad who is aging and losing mobility … he can’t believe it! 🙂
Le mystérieux fascia! Apparemment n’a pas de forme particulière, ferme, fibreux,”goopy” caché dans la membrane autour de la cellule du muscle ou groupe de musculaire .
Très instructif , intéressant à étudier et surtout à localiser.
Great article. I’m a psychotherapist also trained in soft tissue therapies and I love the interconnectivity of mind-body work
Fantastic article. I love the explanation of how it does not need to hurt to work!
Loved this! Thank you for giving such a great overview of our body’s fascial system, so fascinating. The pdf will be so helpful, thank you!
I really enjoyed this in-depth description of the “up to date” fascia information. Esp loved the analogy to the “force”–this made it clear and easy to understand. also found it insightful that foam rolling is not changing the fascia but is still important in giving the body an increase in ROM
This is an excellent Fascia 101 and beyond. I love that this is continuously updates with new information. Thank you for providing an informative and easy to understand explanation of fascia that I can point my students to when they want more information than I can provide in our short classes together. ( I also love your Star Wars reference and the image of not bullying our tissues!)
Excellent information. Another keeper. Learning about the body we live in is fascinating and so educational.
Love learning about fascia. Thank you for this!
The complexity and mystery of fascia explained so beautifully in this article describes seemingly segmented tissues within a working system. However, since all fascia throughout the body IS connected, it evokes the idea of an enormous living organism that holds a sort of invisible role underneath the superficial layers, such as does the mushroom platelets that all connect together under the forest’s rich soil. Mushrooms are considered to be the largest living organism and connect together over hundreds and hundreds of miles and communicate across these vast distances. Fascia seems to work similarly, providing structure and textured to fit specific body parts and functions. Mushrooms actually take on the texture of the terrain they grow on and function as support systems for trees and other living organisms that inhabit a particular space. Given these correlates, and considering the idea fascia compared to the Jedi force presented at the beginning of this article, it seems to point to shapeshifting qualities in the structures that both fascia and mushrooms embody, and the mind blowing communication skills that each of these mysterious systems possess. Great article!!!
I first learn about fascia from the Science of Rolling training, it opened my mind to a new world. The tools and techniques help relieve tensions in my body on a daily basis.
Love this article…concise and easy to understand. I’m going to share it with our students in Yoga Teacher Training.
Excellent Post!
Excellent in depth article. Great use of the corroborating videos. Downloaded the PDF to keep as reference.
Wow, all the things fascia! What a well written and updates discussion about fascia, the layers, the function, and how to interact with it. I love the imagery of fascia specifically the idea of the body being like a solar system all interconnected with different planets along the fascial lines.
The videos were super practical information. Loved the “fuzz” concepts
Great article!
What a perfect article – full of content, recipes, fact and more! I look forward to directing more clients to this article and to an expanded understanding of their body!
Extremely informative article. Dr. Hedley’s research is incredible and I am so thankful to have found him through YTU!
This article is incredible! So much info, and so well thought out and organized. You are amazing….thank you!
Terrific article! Thank you!
Thank you for your work on this and for sharing it. Great content. I love fascia!
Such a fabulous article! It’s often difficult to describe the work I facilitate with The Roll Model Method. I want to reread this daily until the words become embedded in my vocabulary. Perhaps if I lie on the balls while I read….?! : ) Thank you for your efforts!
Thanks for all the great info!
Thanks for this deep and super complete article, saving it for reference
Myofacia as well ozone layer o la capa de ozono son tan importantes para la vida que en caso intoxicarlas o ahogarlas con la contaminación y el sedentarismo, entiendase este cómo falta de atención y cuidados, se atrofia y deja de funcionar adecuadamente.